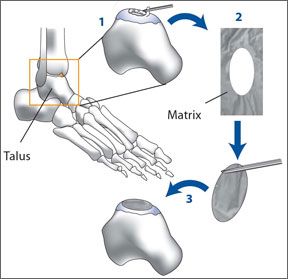
If you have advanced arthritis in the ankle and havent responded to traditional treatment, you may be a candidate for either of two relatively new procedures. One is called autologous chondrocyte implantation (ACI), the other is called matrix-induced autologous implantation (MACI), and both are supported by a growing body of clinical evidence. In the ACI procedure, the surgeon first uses arthroscopic surgery to identify the area of damage, then removes cartilage cells from the ankle or even the knee, and those cells are multiplied in a laboratory for four to six weeks. Once the cells are grown, another surgical procedure-called an osteotomy-is performed to implant the cells.
To continue reading this article or issue you must be a paid subscriber.
Sign in