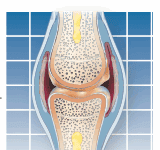
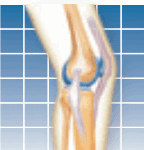
At four months after surgery, it's not unusual to continue to have soreness in the knee that was operated on. This is a result of the increasing intensity of rehabilitation exercises, which put a tremendous amount of stress on muscles that have not been used for some time. Joint replacement surgery is the last step in treatment for arthritis. By the time a person has surgery, other treatments have failed to help and the condition usually has been going on for a long time. Pain and stiffness probably limited your mobility and your muscles became deconditioned. These muscles will be sore until you restore their tone. And that can take some time.
To continue reading this article or issue you must be a paid subscriber.
Sign in