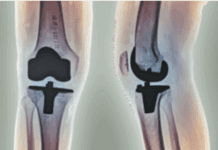
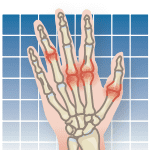
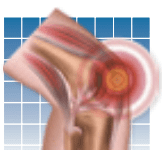
Walking often tops the list of effective ways to get exercise. In fact, the Arthritis Foundation recently launched a campaign to inform people about how walking and other activities can help reduce pain, increase mobility, and slow arthritis progression. But walking isnt easy for everyone. "A number of conditions can cause leg pain that makes walking difficult-and most often, they occur in people who are at risk for developing osteoarthritis or who have already been diagnosed," says Chad Deal, MD, Head of the Center for Osteoporosis and Metabolic Bone Disease at Cleveland Clinic. "Its important to uncover and treat these conditions because they can interfere with your ability to be active and thwart efforts to lose weight, halt progression of osteoarthritis, or prevent it altogether."
To continue reading this article or issue you must be a paid subscriber.
Sign in