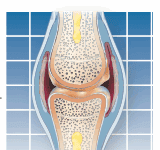
Many medications are available to decrease the joint pain associated with osteoarthritis (OA) and rheumatoid arthritis (RA), as well as the inflammation associated with RA and other types of inflammatory arthritis. The upside of having so many options is that its very likely that you will find a pain medication that works for you. However, making the right choice isnt as simple as you might think. You also need to know about side effects, how the medication interacts with other drugs you may be taking, and how your health status comes into play, says Daniel Mazanec, MD, Associate Director, Cleveland Clinic Center for Spine Health.
To continue reading this article or issue you must be a paid subscriber.
Sign in